
Psoriasis
Psoriasis (pronounces sur-eye-ah-sis) is a skin condition that causes a rash that has itchy and scaly or flaky patches of skin across the body, but can most often be found on the knees, elbows, trunk and scalp.
What is Psoriasis?
Psoriasis is due to inflammation in the skin. Psoriasis is not contagious and cannot be ‘caught’ from someone else. It is pretty common and affects around 1-2% of the population, which means there is probably someone else you know who also has psoriasis.
Psoriasis can develop at any age – affecting babies through to adults – but the most common time for it to come on is in the teens and twenties. It can come and go throughout your life, which is why sometimes it is called chronic plaque psoriasis.
Psoriasis varies from person to person, both in severity and how it responds to treatment. There is unfortunately no cure for psoriasis, but there are many treatment options available to help; the specific type used will depend both on how bad the psoriasis is, and where it’s located on the body.
It can obviously still be depressing to hear that your psoriasis is most likely going to be a life-long thing, but this doesn’t mean that it will always be active, or that it can’t be controlled. If you are struggling to deal with having psoriasis, speak to your doctor, parent or caregiver, or check out our support pages to see where you can access support yourself.
There are several different types of psoriasis, but two are more common in children and young people:
- Chronic plaque psoriasis
- Guttate psoriasis
Chronic plaque psoriasis
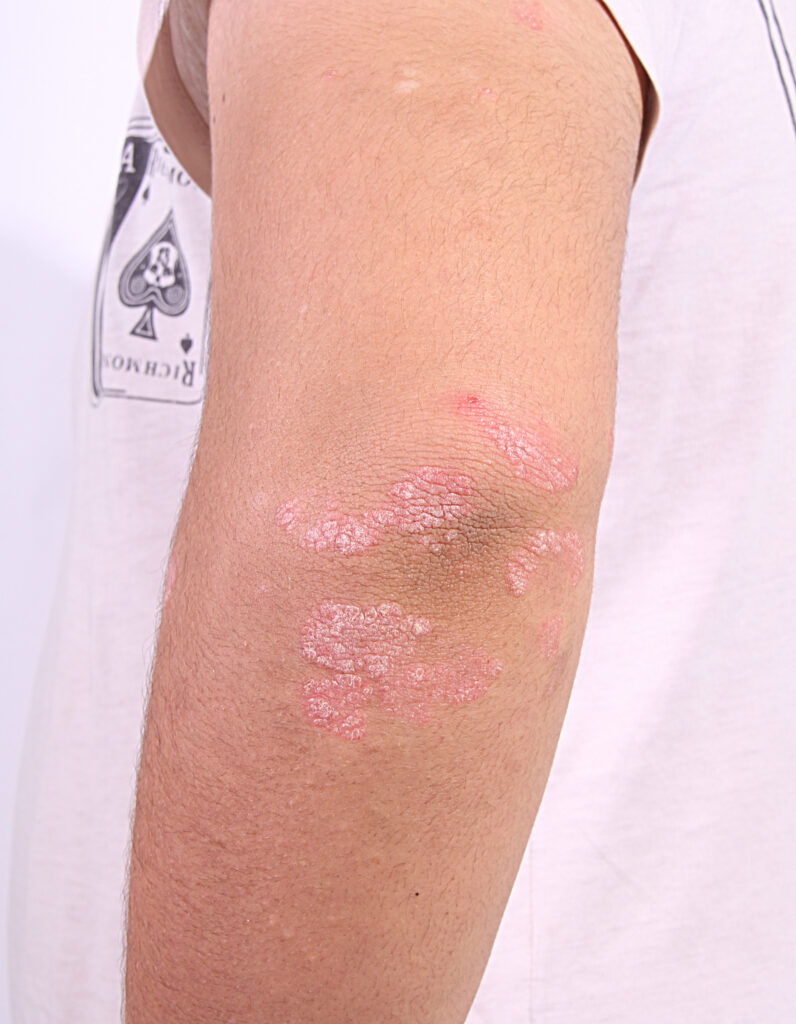
Chronic plaque psoriasis: This is the most common type, and is often just called psoriasis. Chronic means the symptoms can come and go at any time throughout life. Areas of the body most often affected are the scalp (in particular behind ears), the elbows and knees, the navel area (around the belly button), and the genital area. A plaque is a raised, red (or dark) and sometimes itchy area. Psoriasis plaques usually have silvery scales on them.
Guttate psoriasis
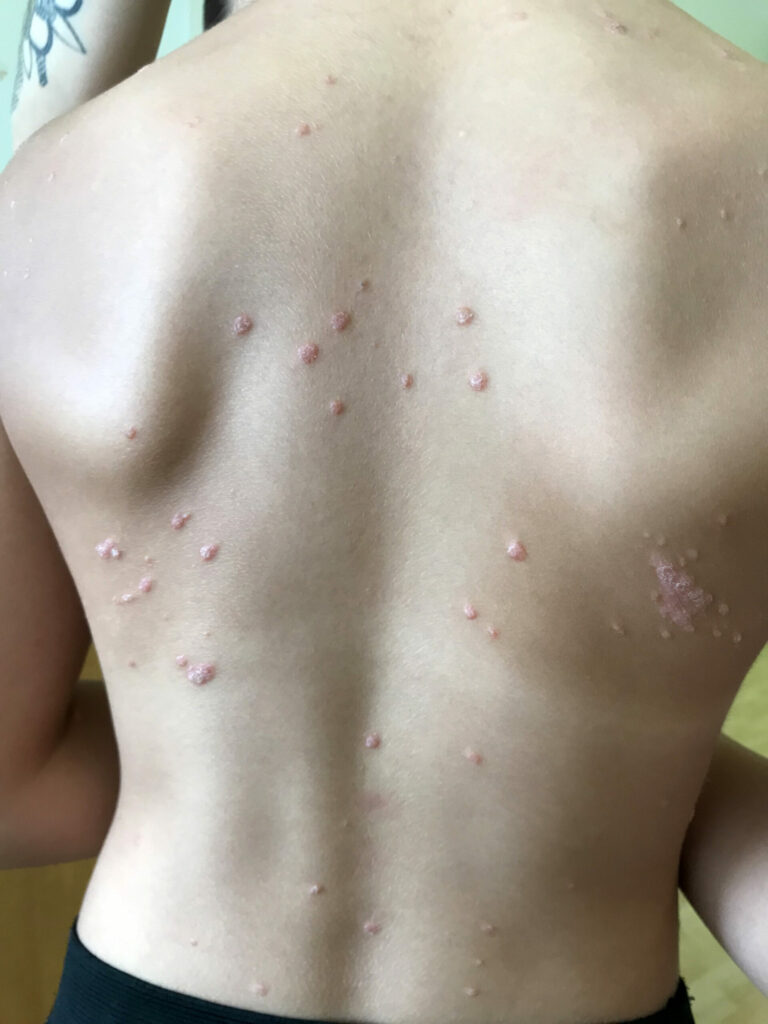
Guttate psoriasis: Small areas of psoriasis mostly on trunk which typically appear just after a throat infection. This may happen as a one-off episode, but can occur repeatedly in some people. It might also make it more likely that you will develop chronic plaque psoriasis.
What are other different types of psoriasis?
Psoriasis can also affect the following areas:
Scalp: Well-demarcated, red plaques with silvery scale. Often itchy and psoriasis can extend onto non-hairy facial and neck skin.
Face: Facial psoriasis is more common in children and young people than adults. Psoriasis also commonly affects the ears canals.
Nails: Causing tiny holes called pitting, thickened or discoloured nails
Skin creases (flexures): For example, armpits, groin, genitals, under breasts. In the flexures, psoriasis is often red smooth and shiny, rather than scaly/flakey.
Joints: Psoriasis can cause joint pain, swelling and stiffness, for example in your hands and feet, lower back, or elbows/knees/hips. If you have any of these symptoms, please speak to your doctor as you may need different treatments.
Treatment
Some people are not bothered by having psoriasis and for these people, sometimes no treatment is needed. Other people are very bothered by their psoriasis, either by how it looks, how it feels or how they think it might affect their friendships and hobbies. There are plenty of effective treatments that can help reduce symptoms and make it less problematic, so having psoriasis should not stop you living your life to the full.
Reduce flakiness and dryness
Psoriasis is often dry and flaky or scaly. It is helpful to use a regular moisturiser (emollient) to reduce the dryness, as this makes psoriasis less itchy. We also think that it can make the active treatments more effective, as they enter the skin more easily when skin is moisturised.
Treat inflammation
Most people with psoriasis use topical steroid ointments or creams. When skin is itchy, red or sore, use your steroid ointment daily. And here’s the important bit: people often don’t use enough topical steroid, or the steroid they use is too weak. This causes some confusion, even among some health workers. This can mean sometimes people aren’t prescribed enough of the right stuff.
Different steroids are used in different parts of the body; milder steroids for the face and sensitive areas, and stronger steroids for thicker skin like knees, elbows, hands and feet. If you aren’t sure which ointment to apply where, ask your doctor, nurse, pharmacist or your parent/caregiver.
Other treatments which can help reduce redness and inflammation in psoriasis included Vitamin D ointments, tacrolimus ointment (“Protopic”), and coal-tar based creams, lotions and shampoos. These treatments are often used “off-licence” in children and young people with psoriasis, but they are recommended in guidelines.
Beyond creams and ointments
If your psoriasis is very widespread, or does not respond to creams and ointments, your doctor or nurse may recommend additional treatments including light treatment (phototherapy), or tablet or injection treatments. These are provided by Dermatology Departments at the hospital. There is more information regarding treatments for more severe psoriasis provided below from the British Association of Dermatologists (BAD).
Useful links for further reading and support
British Association of Dermatologists - Psoriasis in children and young people
British Association of Dermatologists - Psoriasis in adults
British Association of Dermatologists - Psoriasis - topical treatments
British Association of Dermatologists - Psoriasis - phototherapy
British Association of Dermatologists - Treatments for moderate or severe psoriasis
PSO Teen
Psoriasis Association
Healthtalk: Psoriasis
National Psoriasis Foundation - American website for psoriasis and psoriatic arthritis
British Association of Dermatologists - Adalimumab
British Association of Dermatologists - Secukinumab
British Association of Dermatologists - Ustekinumab
Get in touch

